
Often confused with general back pain, Sciatica is usually caused by a compressed nerve in the lower spine. According to experts’ estimate, up to 40 percent of people will experience sciatica at least once in their life. Dr S. Karunagaran, Consultant Orthopedics, Spine Surgeon, Specialist in Joint Replacement & Sports Medicine at Wellkin Hospital, explains the causes, risk factors and most importantly, the treatment of sciatica.
 Sciatica, explains Dr S. Karunagaran, is a term used to describe back or buttock pain radiating to either one or both lower limbs, which can be caused by an array of problems affecting the sciatic nerve. “The sciatic nerve is a large nerve that originates in the lower back and runs down the back of each leg. When the sciatic nerve is irritated, inflamed, compressed or injured, it can cause pain in the lower back that radiates to the hip, buttocks, and the lower limb. In some patients, it can be very severe affecting their ability to sit, stand or walk. In very severe cases, there can be loss or disturbances in sensation of the legs or weakness in the legs.”
Sciatica, explains Dr S. Karunagaran, is a term used to describe back or buttock pain radiating to either one or both lower limbs, which can be caused by an array of problems affecting the sciatic nerve. “The sciatic nerve is a large nerve that originates in the lower back and runs down the back of each leg. When the sciatic nerve is irritated, inflamed, compressed or injured, it can cause pain in the lower back that radiates to the hip, buttocks, and the lower limb. In some patients, it can be very severe affecting their ability to sit, stand or walk. In very severe cases, there can be loss or disturbances in sensation of the legs or weakness in the legs.”
He states that sciatica affects people mostly aged 30 and above. “An increasing number of people are suffering from sciatica all over the world, which is mainly due to our lifestyle, bad sitting habits associated with long working hours or lack of exercise. Women may be more likely to develop the problem during pregnancy because of pressure on the sciatic nerve from the developing uterus. Elderly people who have degenerative spine problems also develop sciatica.”
What are the symptoms of sciatica and how is it diagnosed? “It can cause pain in the lower back that spreads to the hip, buttocks, and leg. The pain can affect one or both legs and may get worse when you sit, cough, or sneeze. The leg may also feel numb, weak, or tingly at times. To diagnose sciatica, a proper physical examination of the patient is required,” states Dr S. Karunagaran.
Risk factors and causes
 The specialist explains that those who are at highest risk of developing sciatica are persons who sit or stand for long hours. “People who do not have a proper sitting posture, for example those who sit with a big wallet in the back pocket or sit on their back instead of their buttock have a higher risk of sciatica. If you bend forward and lift heavy weights on a regular basis, you are also at an increased risk. Obesity is another major risk factor.”
The specialist explains that those who are at highest risk of developing sciatica are persons who sit or stand for long hours. “People who do not have a proper sitting posture, for example those who sit with a big wallet in the back pocket or sit on their back instead of their buttock have a higher risk of sciatica. If you bend forward and lift heavy weights on a regular basis, you are also at an increased risk. Obesity is another major risk factor.”
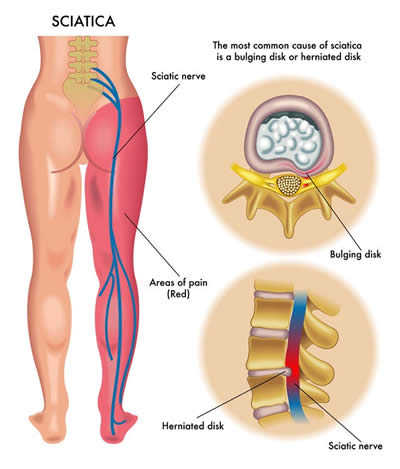
Regarding causes, he utters that the most common one is a herniated disk. “Disks act like shock absorbers between the vertebral body of your spine. With age, these disks tend to lose their compressibility and become vulnerable to injury. The gel-like center of the disk protrudes outside of the outer layer of the disk and compresses against the nerves exiting the spinal cord. In older people, the vertebral column becomes degenerative due to the natural wear and tear causing narrowing of the spinal canal and compression of the sciatic nerve.”
He underlines also that, in rare cases, “sciatica may result from tumors growing within or along the spinal cord or sciatic nerve. These tumors tend to press against the sciatic nerve. The piriformis muscle is a muscle found deep inside the buttocks which can also cause compression on the nerve. Other causes of sciatica include inflammation, infection, or injury, such as a fracture of the spinal column. Any condition that puts pressure on the sciatic nerve can cause sciatica.”
Prevention and treatment
When it comes to treatment for sciatica, Dr S. Karunagaran says that patients can have pain relief with over-the-counter pain medications such as Paracetamol or NSAIDS. “Patients who have severe pain can benefit from an admission in a hospital or clinic for intravenous pain medications. For patients who have persisting pain for more than 4 to 6 weeks, your doctor may opt for an epidural infiltration.”
However, he highlights, “if the pain is still not subsiding, then your doctor might propose surgery. There are different ways of doing surgery on a herniated disk, but generally the goal of the surgery is to remove all compressions on the nerve. The surgical procedure is very safe and can now be done with an added security such as a nerve monitoring device. In some patients, the surgery can be done by minimally invasive technique. Most patients are able to walk in less than one day after surgery and they can be discharged from the hospital or clinic within three days,” he explains.
Can sciatica be completely cured? In most cases, states Dr S. Karunagaran, “the symptoms associated with sciatica will subside with conservative treatments with pain medications and physiotherapy. In more severe cases, the patients will require surgery to decompress the spinal cord and nerves. Most patients undergoing surgery will be cured.” He adds that there are home remedies for relief. “There are steps that can be taken at home to help prevent or decrease the pain. Ice packs or heating pads can be placed over lower back for about 20 minutes every 3-4 hours. You can experiment to see which one works best for you. Furthermore, doing regular core strengthening exercises can also help to prevent sciatica. If you already have sciatica, then it is always good to take small walks instead of staying in bed because motion helps with inflammation and pain.”
Moreover, he trusts that prevention is always better than cure. “Anyone can take measures to prevent sciatica. The most important is to maintain a healthy lifestyle with a good body weight, avoiding sitting for long periods of time, especially on low sofas or stand for extended stretch of time.
Doing lower back strengthening exercises can also help to prevent sciatica. It is always good to see a physiotherapist who can teach you how to do exercises properly. While your sciatica is healing, it is good to remain active, to help reduce pain and inflammation. Practicing other types of exercises such as tai chi or yoga can help stabilize the affected area and strengthen your core.” Regarding follow-up for sciatica, he trusts that in cases such as back pain or pain radiating down the legs will subside on its own with some pain medications, so no follow-up is required. But, he underlines, “if the pain is not subsiding with pain medications and physiotherapy, it is advisable to see a spine surgeon who can ask for an MRI to determine the cause of the pain. He will then accordingly give a follow-up.”
 J'aime
J'aime













